Understanding Pulmonary Hypertension Causes, Symptoms, Treatments
Pulmonary hypertension is high blood pressure in the arteries of the lungs that increases strain on the right side of the heart. This article explains how PH develops, common signs and risks, and summarizes diagnostic approaches and treatment options currently available in the United States.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
What is Pulmonary Hypertension and Its Impact on Heart and Lung Function?
Pulmonary hypertension (PH) involves elevated blood pressure within the pulmonary arteries, which are the blood vessels responsible for carrying deoxygenated blood from the heart to the lungs. Unlike systemic hypertension, which affects the body’s main arteries, PH specifically targets the lung’s vascular system. When the arteries in the lungs narrow, stiffen, or become blocked, the right side of the heart must exert more force to pump blood through them. This continuous overexertion can cause the right ventricle of the heart to become enlarged and less efficient over time, a condition known as right heart failure. The lungs’ ability to effectively exchange oxygen and carbon dioxide is also compromised, leading to various symptoms and reduced physical capacity.
Primary Causes and Risk Factors of Pulmonary Hypertension in the United States
Pulmonary hypertension is categorized into several groups based on its underlying causes. Group 1, known as pulmonary arterial hypertension (PAH), is often idiopathic (without a known cause), heritable, or associated with certain conditions like connective tissue diseases (e.g., scleroderma, lupus), congenital heart disease, or HIV infection. Group 2 PH is caused by left-sided heart disease, which is a very common cause of PH in the United States, as the left side of the heart struggles to pump blood effectively, leading to a backup of pressure in the lungs. Group 3 PH is associated with lung diseases and/or hypoxia, such as chronic obstructive pulmonary disease (COPD), interstitial lung disease, or sleep apnea. Group 4 PH is due to chronic thromboembolic pulmonary hypertension (CTEPH), resulting from blood clots that have not dissolved in the lungs. Group 5 PH includes cases with unclear or multifactorial mechanisms. Risk factors can include genetic predispositions, exposure to certain drugs or toxins, and existing cardiovascular or respiratory conditions.
Recognizing the Symptoms of Pulmonary Hypertension
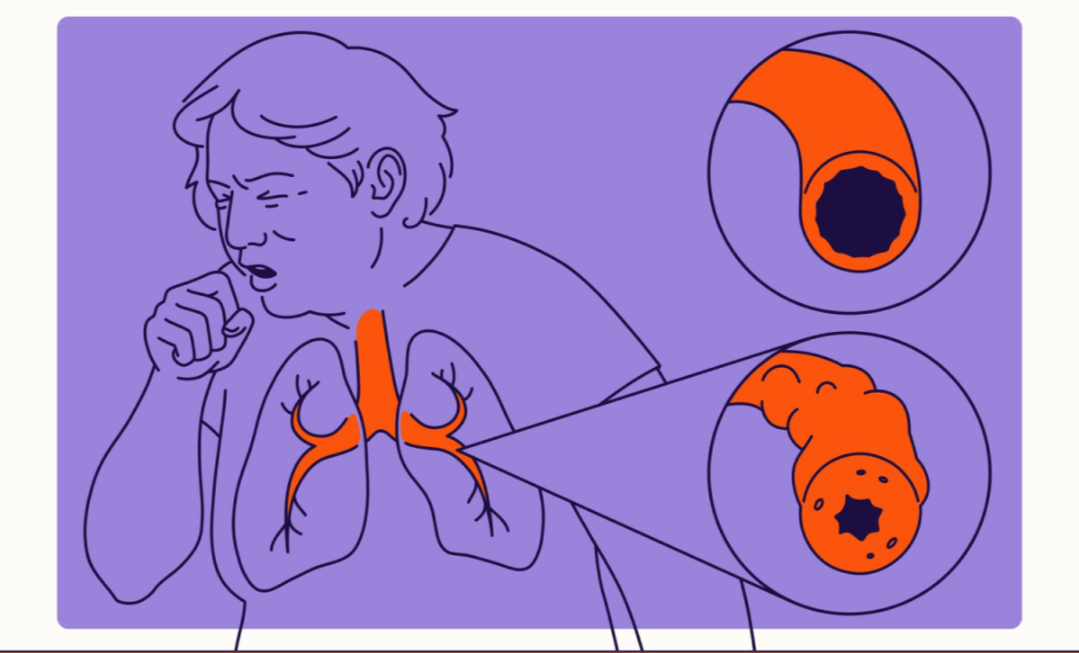
Symptoms of pulmonary hypertension often develop gradually and can be mistaken for other, less serious conditions, making early diagnosis challenging. Common indicators include shortness of breath, particularly during physical activity, which may progress to occurring even at rest. Fatigue and weakness are also prevalent, as the heart works harder and oxygen delivery to the body is impaired. Other symptoms can include chest pain or pressure, dizziness or fainting spells (syncope), especially with exertion, and swelling in the ankles, legs, or abdomen due to fluid retention. Some individuals may also experience a bluish tint to their lips or skin (cyanosis) or a racing heartbeat. If these symptoms are experienced, seeking medical evaluation is important.
Diagnosis of Pulmonary Hypertension in US Clinical Settings
Diagnosing pulmonary hypertension typically involves a comprehensive approach, beginning with a detailed medical history and physical examination. Initial tests often include an electrocardiogram (ECG) to check heart rhythm and strain, a chest X-ray to look for lung or heart abnormalities, and an echocardiogram to assess heart structure and function, including estimates of pulmonary artery pressure. A definitive diagnosis of PH, particularly PAH, usually requires a right heart catheterization. This invasive procedure directly measures the pressure in the pulmonary arteries and the right ventricle, providing precise information about the severity of the condition. Additional tests like pulmonary function tests, blood tests, CT scans, and ventilation-perfusion (VQ) scans may be used to identify underlying causes or rule out other conditions.
Overview of Medical Treatments for Pulmonary Hypertension
While there is currently no cure for pulmonary hypertension, various medical treatments aim to manage symptoms, improve quality of life, and slow the progression of the disease. Treatment strategies are tailored to the specific type and severity of PH. For pulmonary arterial hypertension (PAH), medications that dilate blood vessels in the lungs are often prescribed. These include prostacyclin analogs, endothelin receptor antagonists, phosphodiesterase-5 inhibitors, and soluble guanylate cyclase stimulators. These drugs can be administered orally, inhaled, or intravenously. For PH caused by left-sided heart disease or lung disease, treatment primarily focuses on managing the underlying condition. Oxygen therapy may be prescribed to alleviate shortness of breath and reduce strain on the heart. In some cases, diuretics are used to reduce fluid retention, and anticoagulants may be given to prevent blood clots. For severe cases, lung transplantation or combined heart-lung transplantation may be considered as a last resort. Regular monitoring by a specialist is essential to adjust treatment as needed.
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Pulmonary hypertension is a challenging condition that requires careful management and ongoing medical care. By understanding its causes, recognizing its symptoms, and adhering to prescribed treatments, individuals can work with their healthcare providers to improve their outlook and maintain a better quality of life. Early diagnosis and a personalized treatment plan are key components in addressing this complex health issue effectively.